
Infection Control and Flooring
The importance of infection control and flooring choices for healthy spaces.
The Covid 19 crisis has underlined the importance of hand hygiene and cleaning protocols for preventing transmission of the virus. It has also highlighted how infection prevention and control (IPC) is essential in healthcare and aged-care settings to stop infections and antimicrobial resistance. In this context, choosing the right floor and wall coverings is crucial to the efficiency of cleaning routines.
For decades, Tarkett has been committed to developing innovative flooring solutions that put people first.
Ensuring patient safety, improving the workplace for medical staff, and making life easier for cleaners with a welcoming, hygienic environment is what we call ‘Tarkett Human-Conscious Design TM’.
It also means helping you make the right choices for healthcare settings.
Our experts can provide guidance on choosing floors that offer excellent support for infection prevention and control in hospitals.
The Role of Infection Control
The spread of infection and antimicrobial resistance (AMR) are major threats to public health. Managing both is a constant challenge for all healthcare facilities.
- 1 in 10 hospital patients is affected by HAI each year and 4 million patients across Europe
- 37,000 deaths are associated with HAI in Europe annually, 70% of which are due to antibiotic-resistant microorganisms called ‘superbugs’
source: World Health Organization
Effective infection prevention and control prevents the spread of healthcare-associated infections (HAI) and antimicrobial resistance.
Multi-resistant bacteria is a major public health threat (rising from 25 to 60% between 1995 and 2005) and could lead to 10 million deaths each year in 2050.
Therefore the overuse of disinfectants and antibiotics could encourage the development of antimicrobial resistance and is suspected of posing a risk to human health.
However, these biocidal products may not be necessary with the correct cleaning protocols in place.
What is IPC ?
Infection prevention and control is a set of measures to prevent the spread of healthcare-associated infections and antimicrobial resistance.
What is an HAI?
Healthcare-associated infections are infections acquired by a patient during his or her hospital stay.
What is AMR?
Antimicrobial resistance is the ability of microorganisms to become resistant to antimicrobial agents such as antibiotics and biocides.
The Key Role of IPC in Hospitals
About 80% of infectious diseases are transmitted by unclean hands touching contaminated surfaces (Source: CDC, Center for Disease Control and Prevention).
Hands and touch surfaces are the most critical factors in infection transmission, which is why keeping them clean is crucial. That makes good hand hygiene and environmental cleaning procedures vital. Both are standard precautions for infection control.
Although there is a lack of evidence on the impact of floors in HAI, as low-touch surfaces they should be selected for their:
- resistance to soiling and picking up dirt
- ease of cleaning and compatibility with disinfection protocols.
Good Environmental Hygiene
1. Choosing the right surfaces is critical
The first requirement for good hospital hygiene is that all surfaces, items and equipment within a healthcare environment are cleanable.
This is why selecting the right materials for floors and walls is crucial.
In low-risk areas such as entrances, offices and service areas, the floor and wall coverings have less impact on IPC, but in clinical areas, they should be selected carefully to make cleaning easy.
Requirements for floors and walls in clinical areas
- Smooth & non-porous surface with minimal joints to prevent dirt build-up (which would favour the growth of microorganisms)
- Watertight installation with perfect coving and hot-welded joints for greater durability
- Resistance to the repeated use of disinfectants such as quaternary ammonium, alcohol, bleach and hydrogen peroxide
- Easy-to-repair material. In case of damage, fix on the spot and reseal without changing the whole floor
2. Defining suitable cleaning protocols
Once the proper surfaces are in place, it is important to define and implement the right cleaning protocols.
Cleaning is the key to efficient IPC
Never forget that the basis of a good protocol is to properly clean all surfaces.
That means dry mopping to remove dust and debris, followed by wet mopping with a detergent to clean.
Floors are low-touch surfaces that rarely come into contact with the hands of patients / residents or healthcare providers. Normally, disinfectant is not required and a thorough clean is sufficient.
Disinfect after cleaning only when needed
In clinical areas and wherever the risk of infection is high or outbreaks occur, disinfection - after an effective clean - will be needed.
However, disinfection without cleaning serves no purpose since most disinfectants lose their effectiveness rapidly in the presence of organic matter.
Furthermore, concerns about the adverse human and environmental health effects of cleaning and disinfectant products have led us to look at the development of “green" cleaning methodologies.
“When it comes to flooring, what matters most is keeping it clean and free from soiling and dirt. Disinfection should be restricted to high-risk areas. There is no benefit to using disinfectants in other zones where they often simply soil the flooring.”
Christine Huddlestone, Senior Health Manager, responsible for cleaning, microbiology technician for 20 years, Douai Hospital, France
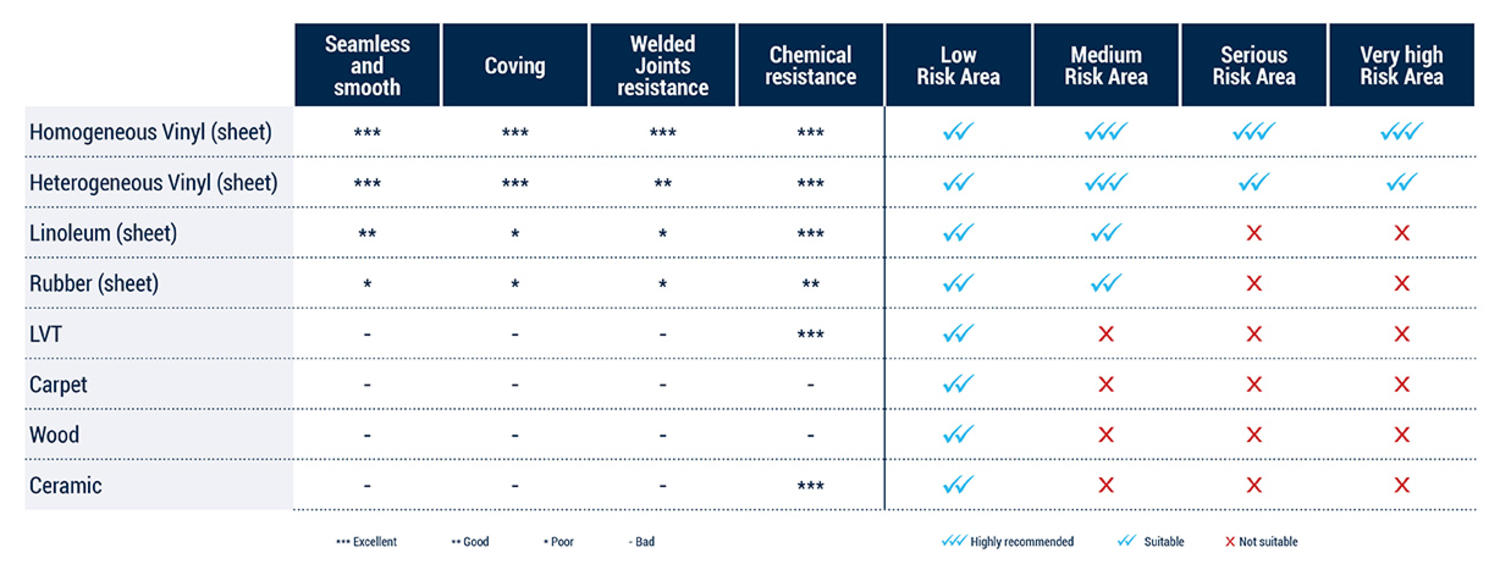
Selecting the Right Floors
While each category of flooring has its own advantages, vinyl rolls represent the best solution for areas with a high risk of infection.
The iQ Ranges for Serious and High-Risk Areas
Our iQ ranges of homogeneous vinyl roll are the best flooring solutions for demanding areas like operating theatres and controlled environments.
- Excellent cleanability - The smooth surface ensures the highest levels of hygiene - proven by the Fraunhofer Institute
- Perfect watertightness - Unmatchable flexibility allowing perfect coving, hot welding and easy repair
- Durable joints - Outstanding seam strength (3 times above standard) preventing split joints
- High chemical resistance - Withstands the strongest disinfectants (quaternary ammonium, alcohol, bleach, hydrogen peroxide etc.)
- Comprehensive solution for floors & walls - Easy to match and heat-weld (ProtectWall and Wallgard) for a fully watertight system
A collection of floor and wall solutions for all areas, whatever their risk level
Hospitals and healthcare facilities feature a wide variety of spaces, from high-traffic zones like entrances to administrative areas, patient rooms, even showers and wet rooms. Each of these spaces has different needs.
We provide a comprehensive collection of coverings for walls and floors to meet the needs of any healthcare environment.
What About Biocides?
Biocides are a controversial topic. Their effectiveness has not been proven and there is a risk of encouraging antimicrobial resistance if used unnecessarily.
- Viruses are different to bacteria. And like antibiotics, antibacterial products are ineffective against viruses.
- On the contrary, the overuse and misuse of antibacterial agents (antibiotics & biocides) may lead to antimicrobial resistance.
- Although a range of antimicrobial-impregnated products (such as surface coatings, paints and curtains) are available, there are, at present, no definitive data to support their effectiveness against healthcare-associated infections.
- Furthermore, standards often used to explain their use and role, such as ISO 22196, are inappropriate for testing antimicrobial surfaces.
.
Tarkett’s position on biocides
We have identified the use of biocides as a major risk to health and the environment and have therefore decided to:
• Stop adding antimicrobials in our flooring production in 2013
• Actively promote the importance of appropriate cleaning
• Recommend the use of disinfectants only where and when necessary
• Promote alternative solutions less reliant on chemicals and disinfectants, such as
microfibre cloths or steam cleaning